Do Oncological Considerations in Malignant Peripheral Nerve Sheath Tumors Differ Among Surgical Specialties? An International Survey
Enrico Martin, MD1, Willem-Bart M. Slooff, MD1, Thijs van Dalen, MD, PhD1, Cornelis Verhoef, MD, PhD2 and J. Henk Coert, MD, PhD1, (1)University Medical Center Utrecht, Utrecht, Netherlands, (2)Erasmus Medical Center, Rotterdam, Netherlands
Background: Malignant peripheral nerve sheath tumors (MPNST) are rare sarcomas and their prognosis remains poor despite curative intents of treatment. Given the origin of MPNSTs, they present among different surgical specialties and considerations for ideal oncological treatment may differ between specialties. This study set out to investigate differences among surgical specialties regarding optimal diagnostics, multimodal treatment, and preoperative functionality considerations.
Methods: Multiple surgical societies (oncologic surgery/hand surgery/peripheral nerve surgery) were asked to distribute this survey online amongst their members. Survey responses were summarized per surgical subspecialty (oncologic surgery/neurosurgery/plastic surgery/other) and differences were analyzed between specialties.
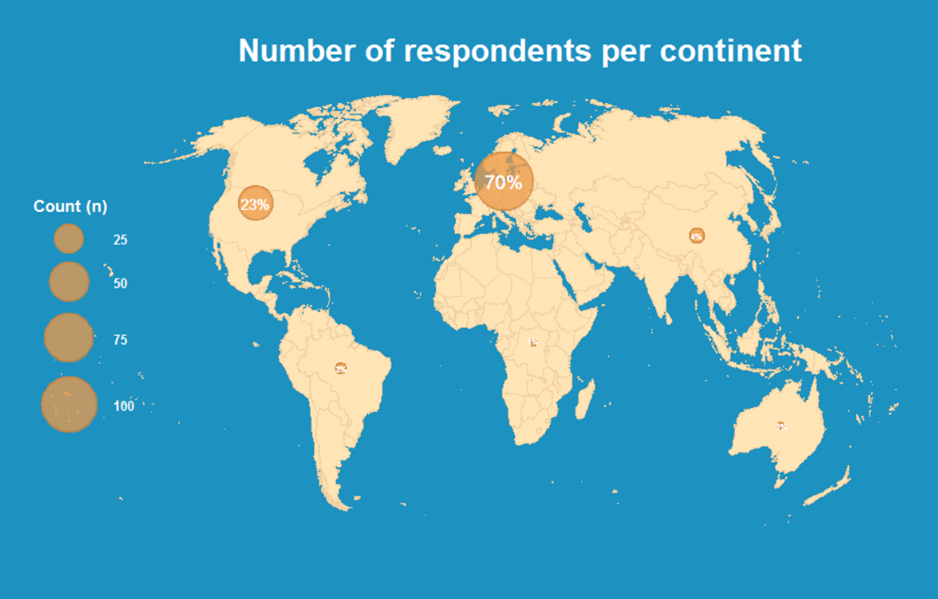
Results: In total, 174 surgeons filled out the survey, including 30 oncologic surgeons, 30 neurosurgeons, 85 plastic surgeons, and 29 other specialists (Figure 1). Oncologic surgeons were most commonly sarcoma-fellowship trained (85.2%, p<0.001). Oncologic surgeons had the highest case load (p<0.001) and more commonly operated truncal sites (p<0.001). Most surgeons distinguished MPNSTs from other sarcomas and benign tumors using both radiology and biopsy (64.6%), most commonly by oncologic surgeons (92.0%, p<0.05). Almost all surgeons used MRI preoperatively (95.4%, p>0.05); a minority of surgeons used a preoperative CT-thorax (24.6%), except oncologic surgeons (64.0%, p<0.001). FDG-PET scans were more commonly used by oncologic surgeons (48.0%) and neurosurgeons (66.7%, p<0.001). Overall, most surgeons preferred core needle biopsies (59.8%), but consensus was more apparent among oncologic surgeons (96.0%). A lack of consensus was present among all subspecialties regarding indications for radiotherapy and chemotherapy, without difference between one another (p>0.05), except for the use of chemotherapy in tumors of 5-10cm (p<0.05). Overall, no preference for adjuvant (35.7%) or neoadjuvant (36.7%) radiotherapy was present, except for oncologic surgeons preferring neoadjuvant administration (72.0%, p<0.05). Preference for chemotherapy sequence was similar across subspecialties (p>0.05). Function was usually considered preoperatively in all subspecialties (65.1%, p>0.05). While rates of neuropathic pain and motor deficit were 40.9% ±22.9% and 36.7% ±25.5% respectively (p>0.05), 42.2% never considered less extensive resections to preserve function. The nerve of origin was usually looked for by all subspecialties (74.1%, p>0.05). A slight minority of surgeons thought that resecting more of the originating nerve might benefit outcomes (47.2%, p>0.05).
Conclusion: A lack of consensus still exists among surgical specialties treating MPNSTs, more so in specialties other than oncologic surgery. Overall, the distribution of opinions was often similar between surgical specialties, while present differences may be due to specialty bias. A multidisciplinary approach remains essential for optimal treatment.
Figure 1
Back to 2020 ePosters